– Policy Brief
Executive summary:
Background
A hidden burden of the covid-19 pandemic is the delay of procedures when intensive care units (ICU) need to be cleared in anticipation for epidemic waves. On April 14th 2021, a number of control measures were lifted in Switzerland, with the potential to increase admissions of COVID-patients in ICUs, and thus limit resources for patients with other conditions. We previously reported on a backlog of an estimated 26,382 patients since the beginning of the covid-19 epidemic in Switzerland (Policy Brief, The double burden of operating near intensive care saturation in Switzerland). Here, following the release of covid-19 control measures we attempt to estimate the additional backlog of patients whose procedures might be delayed because of a 3rd epidemic wave. This analysis accounts for variations in length of stays in ICU for multiple categories of pathologies as well as the proportion of elective procedures for each of these pathologies. Our estimates are based on yearly reports of ICU occupancy provided by the Swiss Society for Intensive Care Medicine (SGI-SSMI). We thank the SGI-SSMI, for their valuable help, and collaboration.
Method
We used projections of ICU occupancy for covid-19 patients from Swiss TPH (Prof. Penny et al) for the period April 20th to September 1st. Three scenarios were considered with regards to vaccination rates. First, an “optimistic” scenario where vaccination could be scaled-up to 50,000 doses per day immediately. The scenario is called “Medium vaccine rollout, expected relax on April 19”. For comparison, current vaccination rates between April 7th to April 14th, were 38,000 doses per day. Therefore, we also considered a second scenario hereafter referred to as “Current vaccination trend”. Projections for this scenario were obtained by averaging projection for ICU occupancy for vaccination rates of 50,000 per day, and 25,000 per day (Penny et al). The third scenario considered was that of very rapid vaccine rollout of 100,000 per day. This scenario would imply multiplying by almost 3 the current pace of vaccination. Projections for ICU occupancy were adjusted such that the first day of projection for April 20th matches the number of covid-19 ICU patients reported in the IES system on the same date.
The proportion of elective procedures were calculated for each category of diagnostic recognized by the SGI-SSMI using records of all patients that attended ICUs in Switzerland between 2018 and 2020 (n = 165,574).
Results
In 2019, 82,064 patients were admitted to intensive care in Switzerland, and ICU bed occupancy was 66%. This pre-covid baseline occupancy corresponds to 578 beds in use – averaging over seasonal variations- out of 875 certified ICU beds reported in the IES system (20th of April 2021). The proportion of patients in ICU for elective procedures was 0.3. The diagnostic associated with the highest proportion of non-urgent elective procedures, and thus likely to be delayed were: R5, Malignant tumor of intra-thoracic organs (74%); R6, Malignant tumor of the respiratory system (72%); M9, Other surgery for metabolic or endocrine diseases, malnutrition, obesity (59%); C9, Other cardiovascular disease such as bypasses, valve, unruptured aortic aneurysms (58%); C5, Aortic Aneurysm (53%), N9, non-urgent neurologic surgery (50%). Patients with urogenital pathologies were removed from the analysis (n<5).
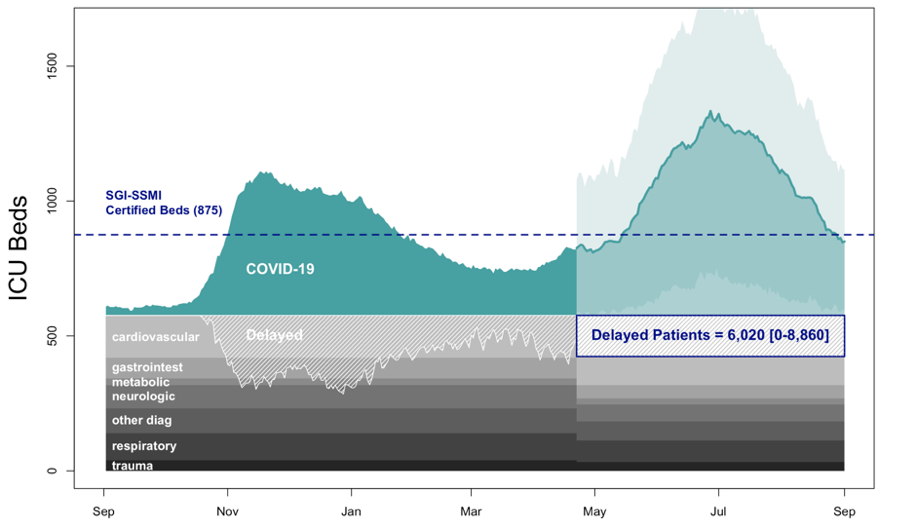
Figure 1A. Current vaccination trends scenario (See methods). ICU Occupancy in Switzerland for vaccination rates between 25,000 and 50,000 doses per day (Methods). Baseline of non-covid patients in 2019 (grey), and covid patients (green), including projections for 3rd wave (light green), and projection uncertainty (mint green).
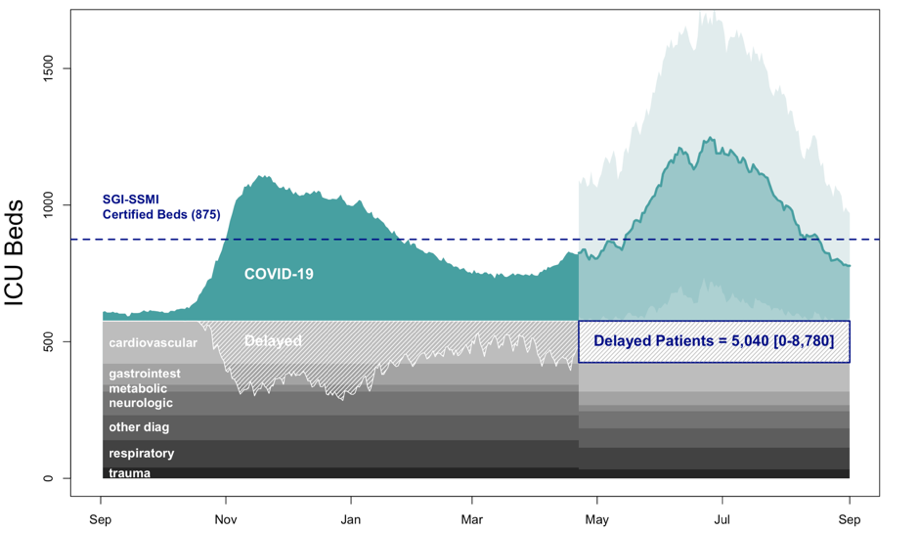
Figure 1B. Optimistic scenario. ICU Occupancy in Switzerland for 50,000 vaccine doses per day. Baseline of non-covid patients in 2019 (grey), and covid patients (green), including projections for 3rd wave (light green), and projection uncertainty (mint green).
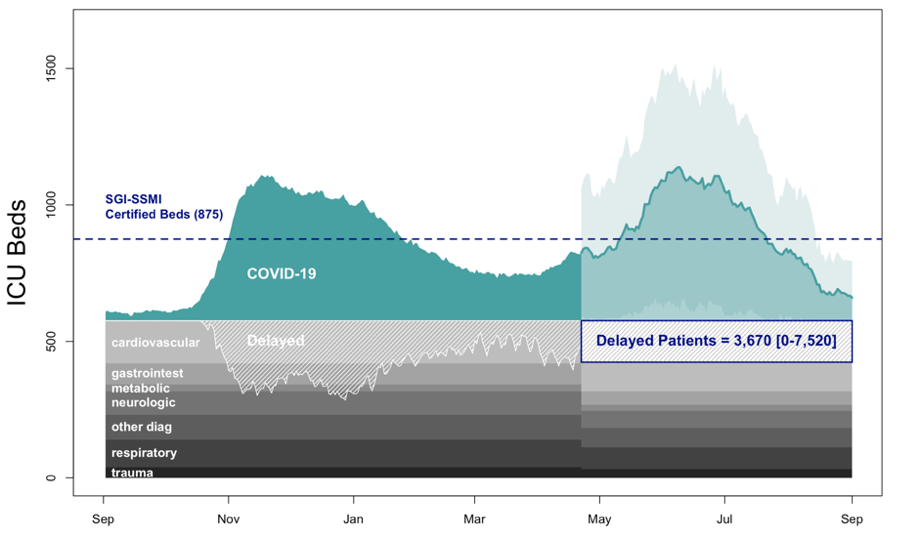
Figure 1C. Fast vaccine rollout. ICU Occupancy in Switzerland for vaccination rates between of 100,000 doses per day. Baseline of non-covid patients in 2019 (grey), and covid patients (green), including projections for 3rd wave (light green), and projection uncertainty.
Under the scenario considered, the cancellation of non-urgent procedures in anticipation for a potential 3rd wave in Switzerland would result in an additional backlog of 6,020 [CI 95% 0-8,780] patients until September 2021 (next 135 days). Considerable uncertainty surrounds these estimates, ranging from no backlog, to the creation of a backlog in excess of 9,000 patients. Upscaling vaccination to 100,000 doses per day would enable to halve the upcoming backlog of patients in ICU.
On current vaccination trends the backlog would include 2,358 [0-3,471] patients with cardiovascular pathologies, 920 [0-1,355] patients with gastrointestinal pathologies, 204 [0-301] patients with metabolic pathologies, 845 [0-1,244] patients with Neurologic pathologies, 838 [0-1,232]patients with other diagnostics, 662 [0-975] patients with respiratory disorder (non-covid), and 192 [0-283] with traumas.
If vaccination could be ramped-up to 50,000 doses/day the backlog would include 1974 [0-3,437] patients with cardiovascular pathologies, 771 [0-1,342] patients with gastrointestinal pathologies, 171 [0-298] patients with metabolic pathologies, 708 [0-1,232] patients with Neurologic pathologies, 701 [0-1221] patients with other diagnostics, 554 [0-965] patients with respiratory disorder (non-covid), and 161 [0-280] with traumas.
If vaccination could be ramped-up to 100,000 doses/day the backlog would include 1,436 [0-2,944] patients with cardiovascular pathologies, 560 [0-1,149] patients with gastrointestinal pathologies, 124 [0-255] patients with metabolic pathologies, 514 [0-1,055] patients with Neurologic pathologies, 510 [0-1,045] patients with other diagnostics, 403 [0-827] patients with respiratory disorder (non-covid), and 117 [0-240]with traumas.
Leaving out all ICU patients with the diagnostics aforementioned would clear a bed capacity of 152 beds per day compared to the baseline occupancy of ICUs by non-covid patients (578) in 2019. However, under the current vaccination trend scenario of our modelled projections, the simulation peak of the 3rd epidemic wave (June 27st), demand for ICU beds is expected to reach 1,182 (accounting cancelled procedures). This will exceed the certified bed capacity (875) by 307 beds. Under this scenario, more than 1 in 3 (40%) covid-19 patients expected to be in ICU would need to be treated outside of ICU, due to limited bed availability. Under the rapid vaccination scenario (100,000) the overflow ICU capacity of certified beds could be limited to 111 beds. Upscaling vaccination, in addition to observance of personal protection measures, would help considerably reduce the risk of negative health impact for patients waiting for procedures that require hospitalization in intensive care.
Date of request: –
Date of response: 21/04/2021
Experts involved: Thomas Van Boeckel, Melissa Penny
Contact persons: thomas.vanboeckel@env.ethz.ch